Disability/Medical Integration Product Helps Streamline the Claims Process
Employer groups that choose both medical coverage with Health Advocacy Solutions (HAS) and disability coverage through Blue Cross and Blue Shield of Montana can take advantage of an integration between the health advocacy and disability teams for a better disability claim experience.
Employees can authorize medical information to be shared between HAS and the disability claim team in order to streamline the disability claim process and arrive at a decision faster. This improved experience allows employees to focus their attention on their treatment and recovery, so they can return to work faster.
What is a Health Advocate?
Employees with medical coverage and HAS have access to a benefits specialist and personal health care resource known as a health advocate. A clinical health advocate serves as a bridge, working with the disability team in the event an employee has a condition that might be best managed with treatment and disability leave.
How Does the Health Advocacy Team Help with Disability Claims?
In the case of a disability, a clinical health advocate can:
- Identify potential eligibility for disability benefits
- Assist with the claim process
- And now, with the employee’s authorization, share medical information directly with the disability team to expedite the review and decision on a claim
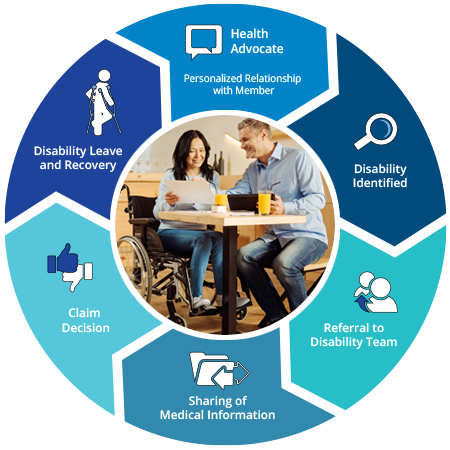
The Circle of Care
By working with a clinical health advocate and sharing information, employees should expect:
- The potential to eliminate the time-consuming exchange of paperwork between employee, provider and claims team
- A significantly faster decision process
- Reduced stress with the assistance of a clinical health advocate through the process
- Improved health outcomes with more personalized attention
What About Complex STD and LTD Claims?
Disability claims that are related to mental and nervous conditions or other complex claims can be managed using an all new clinical round table review made up of clinical resources from the HAS team, the Disability team and the Behavioral Health team. This approach brings together the experience of clinical resources to focus on managing complex disability claims and helping the disabled employee recover and return to work.
What is the Benefit to the Employer?
With dedicated support and ongoing management of health conditions, employees can stay healthier, which reduces absenteeism. In the case of a disability, employees can focus on their recovery and return to work faster.
Employers that choose to offer medical coverage with HAS and integrated disability are providing their employees with a deeper level of support for their overall health and wellness, making it a valuable benefit in attracting and retaining talent.
How Does a Customer Get Started?
Groups that want to offer this integration to their employees can engage their account manager to begin the implementation process which takes approximately 4 months.
For more information, contact your sales representative.
Disability and Health Advocacy Solutions Integration Broker/Employer Group Flyer
Medical and Dental products are offered by Blue Cross and Blue Shield of Montana, a division of Health Care Service Corporation, a Mutual Legal Reserve Company, an Independent Licensee of the Blue Cross and Blue Shield Association. Life, Disability, Critical Illness, Accident and Vision products issued by Dearborn Life Insurance Company, 701 E. 22nd St. Suite 300, Lombard, IL 60148. Blue Cross and Blue Shield of Montana is the trade name of Dearborn Life Insurance Company, an independent licensee of the Blue Cross and Blue Shield Association.
